Post op complications are a risk everyone must consider when planning surgery. While there is no surefire way to prevent 100% of post op complications, there are ways to reduce your risk of some of these issues.
What are some post op complications I should be aware of?
Fever
 Fever is a vague symptom that can be normal and even expected after surgery; up to 90% of surgical patients have a low grade fever due to the body’s inflammatory response to injury. However, it can also be a sign of something more serious, such as atelectasis (collapse of small air sacs in the lung), urinary tract infection (especially if you had a foley catheter placed for surgery), wound infection, or blood clots.
Fever is a vague symptom that can be normal and even expected after surgery; up to 90% of surgical patients have a low grade fever due to the body’s inflammatory response to injury. However, it can also be a sign of something more serious, such as atelectasis (collapse of small air sacs in the lung), urinary tract infection (especially if you had a foley catheter placed for surgery), wound infection, or blood clots.
A slight fever in the first two days after surgery is most likely nothing to be concerned about. However, if you develop other symptoms or if your fever worsens or persists, contact your doctor. The best way to deal with post-op fever is by preventing the more serious causes, as described in the following.
Atelectasis (collapse of air sacs in the lung)
 Atelectasis can stem from the effects of anesthesia as well as a decrease in physical activity and shallow breathing after surgery. It can lead to pneumonia and other more serious respiratory complications. Depending on your procedure, coughing and deep breathing exercises may cause discomfort, but they play an important role in your recovery. Splinting (holding a pillow firmly against your incision) and adequate pain control can help make deep breathing less painful, especially if your surgery involved your chest or upper body.
Atelectasis can stem from the effects of anesthesia as well as a decrease in physical activity and shallow breathing after surgery. It can lead to pneumonia and other more serious respiratory complications. Depending on your procedure, coughing and deep breathing exercises may cause discomfort, but they play an important role in your recovery. Splinting (holding a pillow firmly against your incision) and adequate pain control can help make deep breathing less painful, especially if your surgery involved your chest or upper body.
You may also be sent home with an incentive spirometer. This is a device you’ll use to help expand your lungs thoroughly and gives a give visual representation of your breathing. Not everyone will need an incentive spirometer but everyone should practice some form of deep breathing and coughing to prevent atelectasis during recovery.
Urinary Retention or UTI
 Urinary retention, or the inability to empty your bladder, can occur as a result of the anesthesia used during surgery. We like to have all our patients empty their bladder prior to being discharged to help avoid this complication. Should you be unable to urinate after surgery, contact your doctor for instructions. Treatment may include the insertion of a urinary catheter for manual drainage or medication to help stimulate the bladder.
Urinary retention, or the inability to empty your bladder, can occur as a result of the anesthesia used during surgery. We like to have all our patients empty their bladder prior to being discharged to help avoid this complication. Should you be unable to urinate after surgery, contact your doctor for instructions. Treatment may include the insertion of a urinary catheter for manual drainage or medication to help stimulate the bladder.
Both urinary retention and the use of urinary catheters can lead to urinary tract infections. Increasing your fluid intake, urinating frequently, and maintaining good personal hygiene can help prevent these issues.
Wound Dehiscence or Infection
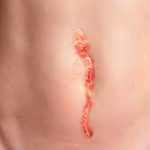 Wound dehiscence is the opening of your incision after surgery. It can be caused by excess strain on the incision, a “popped” stitch, or poor tissue quality at the surgical site. If the opening is minor, you may not have to do anything other than keep the area clean and dry. A larger opening may require dressing changes or a secondary procedure to ensure your wound is closed adequately.
Wound dehiscence is the opening of your incision after surgery. It can be caused by excess strain on the incision, a “popped” stitch, or poor tissue quality at the surgical site. If the opening is minor, you may not have to do anything other than keep the area clean and dry. A larger opening may require dressing changes or a secondary procedure to ensure your wound is closed adequately.
You can help prevent dehiscence by splinting or supporting your incision during position changes, avoiding excess force or friction in the area, following your doctor’s recommendations for activity limitations, and maintaining a healthy diet to promote wound healing.
Wound infection can occur for a number of reasons but is best treated quickly. Signs of infection include excess redness, pain, and swelling; pus or excessive drainage; swollen lymph nodes; fever; odor; or delayed healing. Call your doctor right away if you think you have a wound infection.
 Treatment can include topical antibiotics such as bacitracin ointment, oral/IV antibiotics, or the need for additional surgery to clean and re-close your wound. Prevention includes keeping your incisions clean, changing your dressings as directed, taking your antibiotics as prescribed, and maintaining good personal hygiene. Never scrape or pick at your healing wounds and always wash your hands well before performing any wound care.
Treatment can include topical antibiotics such as bacitracin ointment, oral/IV antibiotics, or the need for additional surgery to clean and re-close your wound. Prevention includes keeping your incisions clean, changing your dressings as directed, taking your antibiotics as prescribed, and maintaining good personal hygiene. Never scrape or pick at your healing wounds and always wash your hands well before performing any wound care.
Blood Clots
Blood clots can form in the larger veins, commonly in the arms or legs; they can also break loose and travel, making them potentially life threatening. However, proper surveillance and preventive techniques can help reduce the risk. We screen every patient with a deep vein thrombosis (DVT) risk assessment tool and certain patients are required to have a pre-op ultrasound of their legs to check for existing blood clots.
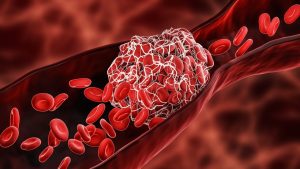
There are also a number of techniques surgeons can use to help reduce the risk of clot formation, including “blood thinners” – anti-thrombotic medications given to help keep blood from clotting; the use of compression or ted hose during and after surgery; and the use of sequential compression devices that massage the calves to keep the blood from pooling.
While recent data call into question these risk reducing techniques for DVTs, the easiest and cheapest form of prevention during recovery is early ambulation. Ambulation, or walking, has several benefits besides blood clot prevention; it also helps promote deep breathing and helps with gas, bloating, and constipation. We want our patients up and walking by the evening of their surgery day, but always follow your surgeon’s instructions for activity limitations.
Written by Jennifer “Coop” Cooper MS, APRN, AGACNP-BC, Sergeant, US Army (veteran)
Click here for the original blog post written by Jennifer Cooper MS, APRN for BuildMyHealth.